|
|
| Linje 28: |
Linje 28: |
| | == '''Sekvenser''' == | | == '''Sekvenser''' == |
| | | | |
| − | <noinclude>This table is used in the following articles:
| + | [[Fil:MRsekvenser.png]] |
| − | *[[Magnetic resonance imaging#Sequences]]
| |
| − | *[[MRI sequences#Overview table]]
| |
| − | *[[Physics of magnetic resonance imaging#Overview of main sequences]].
| |
| − | | |
| − | </noinclude>{{#if:{{{header|}}}|{{{header}}}| }}{{#if:{{{Link-to-main|}}}|{{Main|MRI sequence}}| }}
| |
| − | {{Edit|Template:Table of MRI sequences}}<br>This table does not include [[MRI_sequences#Uncommon_and_experimental_sequences|uncommon and experimental sequences]].
| |
| − | | |
| − | {|class="wikitable"
| |
| − | |-
| |
| − | ! Group !! Sequence !! [[Abbreviation|Abbr.]] !! Physics !! Main clinical distinctions !! Example
| |
| − | |-
| |
| − | |rowspan=3| [[Spin echo]] || [[Magnetic_resonance_imaging#T1_and_T2|T1 weighted]] || '''T1''' || Measuring [[spin–lattice relaxation]] by using a short [[repetition time]] (TR) and [[echo time]] (TE)
| |
| − | |
| |
| − | * Lower signal for more water content, <ref name=wisconsin>{{cite web|url=https://www.radiology.wisc.edu/education/med_students/neuroradiology/NeuroRad/Intro/MRIintro.htm|title=Magnetic Resonance Imaging|publisher=[[University of Wisconsin]]|accessdate=2016-03-14}}</ref>as in [[edema]], [[tumor]], [[infarction]], [[inflammation]], [[infection]], hyperacute or chronic [[hemorrhage]] <ref name=johnson>{{cite web|url=http://www.med.harvard.edu/aanlib/basicsMR.html|author=Keith A. Johnson|title=Basic proton MR imaging. Tissue Signal Characteristics|accessdate=2016-03-14|publisher=[[Harvard Medical School]]|deadurl=yes|archiveurl=https://web.archive.org/web/20160305000107/http://www.med.harvard.edu/aanlib/basicsMR.html|archivedate=2016-03-05|df=}}</ref>
| |
| − | *High signal for [[fat]]<ref name=wisconsin/><ref name=johnson/>
| |
| − | *High signal for [[Paramagnetism|paramagnetic]] substances, such as [[MRI contrast agent]]s<ref name=johnson/>
| |
| − | Standard foundation and comparison for other sequences.
| |
| − | | [[File:T1-weighted-MRI.png|100px]]
| |
| − | |-
| |
| − | | [[Magnetic_resonance_imaging#T1_and_T2|T2 weighted]] || '''T2''' || Measuring [[spin–spin relaxation]] by using long TR and TE times.
| |
| − | |
| |
| − | *Higher signal for more water content.<ref name=wisconsin/>
| |
| − | *Low signal for fat.<ref name=wisconsin/>
| |
| − | *Low signal for [[Paramagnetism|paramagnetic]] substances.<ref name=johnson/>
| |
| − | Standard foundation and comparison for other sequences.
| |
| − | | [[File:Normal axial T2-weighted MR image of the brain.jpg|100px]]
| |
| − | |-
| |
| − | |[[MRI sequence#PD|Proton density weighted]] || '''PD''' || Long [[repetition time|TR]] (to reduce T1) and short [[echo time|TE]] (to minimize T2)<ref>[https://books.google.se/books?id=1pV35-skfkwC&pg=PA292 Page 292] in: {{cite book|title=Principles and Applications of Radiological Physics|author=Martin Vosper, Donald Graham, Paul Cloke|edition=6|publisher=Elsevier Health Sciences|year=2011|isbn=9780702046148}}</ref>
| |
| − | | [[Arthropathy|Joint disease]] and injury.<ref>{{cite web|url=https://radiopaedia.org/articles/mri-sequences-overview|title=MRI sequences (overview)|author=Jeremy Jones and Prof Frank Gaillard et al.|website=[[Radiopaedia]]|accessdate=2017-01-13}}</ref>
| |
| − | *High signal from [[Tear of meniscus|meniscus tears]]<ref name="LefevreNaouri2016">{{cite journal|last1=Lefevre|first1=Nicolas|last2=Naouri|first2=Jean Francois|last3=Herman|first3=Serge|last4=Gerometta|first4=Antoine|last5=Klouche|first5=Shahnaz|last6=Bohu|first6=Yoann|title=A Current Review of the Meniscus Imaging: Proposition of a Useful Tool for Its Radiologic Analysis|journal=Radiology Research and Practice|volume=2016|year=2016|pages=1–25|issn=2090-1941|doi=10.1155/2016/8329296}}</ref> (pictured)
| |
| − | | [[File:Proton density MRI of a grade 2 medial meniscal tear.jpg|100px]]
| |
| − | |-
| |
| − | | [[Gradient echo]] || [[Steady-state free precession imaging|Steady-state free precession]] || '''SSFP''' || Maintenance of a steady, residual transverse magnetisation over successive cycles.<ref name=Luijkx>{{cite web|url=https://radiopaedia.org/articles/steady-state-free-precession-mri-2|title=Steady-state free precession MRI|author=Dr Tim Luijkx and Dr Yuranga Weerakkody|website=[[Radiopaedia]]|accessdate=2017-10-13}}</ref> || Creation of [[Cardiac magnetic resonance imaging|cardiac MRI]] videos (pictured).<ref name=Luijkx/> || [[File:Four chamber cardiovascular magnetic resonance imaging.gif|100px]]
| |
| − | |-
| |
| − | |rowspan=3| Inversion recovery
| |
| − | | Short tau inversion recovery || '''STIR''' || Fat suppression by setting an [[inversion time]] where the signal of fat is zero.<ref>{{cite web|url= https://radiopaedia.org/articles/short-tau-inversion-recovery|title=Short tau inversion recovery|author=Mohammad Taghi Niknejad|website=[[Radiopaedia]]|accessdate=2017-10-13}}</ref>
| |
| − | | High signal in [[edema]], such as in more severe [[stress fracture]].<ref>{{cite web|url=http://www.radiologyassistant.nl/en/p4615feaee7e0a/stress-fractures.html|title=Stress fractures|website=[[Radiopaedia]]|author= Ferco Berger, Milko de Jonge, Robin Smithuis and Mario Maas|accessdate=2017-10-13}}</ref> [[Shin splints]] pictured: || [[File:Shinsplint-mri (crop).jpg|70px]]
| |
| − | |-
| |
| − | | [[Fluid attenuated inversion recovery]] || '''FLAIR''' || Fluid suppression by setting an inversion time that nulls fluids. || High signal in [[Lacunar stroke|lacunar infarction]], [[Multiple sclerosis|multiple sclerosis (MS) plaques]], [[Subarachnoid hemorrhage|subarachnoid haemorrhage]] and [[meningitis]] (pictured).<ref name=":0">{{Cite web|title = Fluid attenuation inversion recoveryg|url = http://radiopaedia.org/articles/fluid-attenuation-inversion-recovery|website = radiopaedia.org|accessdate = 2015-12-03}}</ref> || [[File:FLAIR MRI of meningitis.jpg|100px]]
| |
| − | |-
| |
| − | | Double inversion recovery || '''DIR''' || Simultaneous suppression of [[cerebrospinal fluid]] and [[white matter]] by two inversion times.<ref name=muzio>{{cite web|url=https://radiopaedia.org/articles/double-inversion-recovery-sequence|title=Double inversion recovery sequence|author=Dr Bruno Di Muzio and Dr Ahmed Abd Rabou|website=[[Radiopaedia]]|accessdate=2017-10-13}}</ref>
| |
| − | | High signal of [[multiple sclerosis]] plaques (pictured).<ref name=muzio/>
| |
| − | | [[File:Axial DIR MRI of a brain with multiple sclerosis lesions.jpg|100px]]
| |
| − | |-
| |
| − | |rowspan=3| [[Diffusion weighted imaging|Diffusion weighted]] ('''DWI''') || Conventional || '''DWI''' || Measure of [[Brownian motion]] of water molecules.<ref>{{cite web|url=https://radiopaedia.org/articles/diffusion-weighted-imaging-1|title=Diffusion weighted imaging|author=Neuro and Dr Usman Bashir|accessdate=2017-10-13|website=[[Radiopaedia]]}}</ref>
| |
| − | | High signal within minutes of [[cerebral infarction]] (pictured).<ref>{{cite web|url=https://radiopaedia.org/articles/ischaemic-stroke|title=Ischaemic stroke|author=Dr Yuranga Weerakkody and Prof Frank Gaillard et al.|website=[[Radiopaedia]]|accessdate=2017-10-15}}</ref>
| |
| − | | [[File:Cerebral infarction after 4 hours on DWI MRI.jpg|100px]]
| |
| − | |-
| |
| − | | [[Apparent diffusion coefficient]] || '''ADC''' || Reduced T2 weighting by taking multiple conventional DWI images with different DWI weighting, and the change corresponds to diffusion.<ref name=hammer>{{cite web|url=http://xrayphysics.com/dwi.html#adc|title=MRI Physics: Diffusion-Weighted Imaging|author=Mark Hammer|website=XRayPhysics|accessdate=2017-10-15}}</ref>
| |
| − | | Low signal minutes after [[cerebral infarction]] (pictured).<ref name="AnFord2011">{{cite journal|last1=An|first1=H.|last2=Ford|first2=A. L.|last3=Vo|first3=K.|last4=Powers|first4=W. J.|last5=Lee|first5=J.-M.|last6=Lin|first6=W.|title=Signal Evolution and Infarction Risk for Apparent Diffusion Coefficient Lesions in Acute Ischemic Stroke Are Both Time- and Perfusion-Dependent|journal=Stroke|volume=42|issue=5|year=2011|pages=1276–1281|issn=0039-2499|doi=10.1161/STROKEAHA.110.610501}}</ref>
| |
| − | | [[File:Cerebral infarction after 4 hours on ADC MRI.jpg|100px]]
| |
| − | |-
| |
| − | | Diffusion tensor || '''DTI''' || Mainly [[tractography]] (pictured) by an overall greater [[Brownian motion]] of water molecules in the directions of nerve fibers.<ref name=radiopaedia-dti>{{cite web|url=https://radiopaedia.org/articles/diffusion-tensor-imaging|title=Diffusion tensor imaging|author=Derek Smith and Dr Usman Bashir|accessdate=2017-10-13|website=[[Radiopaedia]]}}</ref>
| |
| − | |
| |
| − | *Evaluating white matter deformation by tumors<ref name=radiopaedia-dti/>
| |
| − | *Reduced [[fractional anisotropy]] may indicate [[dementia]]<ref name="ChuaWen2008">{{cite journal|last1=Chua|first1=Terence C|last2=Wen|first2=Wei|last3=Slavin|first3=Melissa J|last4=Sachdev|first4=Perminder S|title=Diffusion tensor imaging in mild cognitive impairment and Alzheimerʼs disease: a review|journal=Current Opinion in Neurology|volume=21|issue=1|year=2008|pages=83–92|issn=1350-7540|doi=10.1097/WCO.0b013e3282f4594b}}</ref>
| |
| − | | [[File:White Matter Connections Obtained with MRI Tractography.png|100px]]
| |
| − | |-
| |
| − | | rowspan=3| [[Perfusion MRI|Perfusion weighted]] ('''PWI''')
| |
| − | | [[Dynamic susceptibility contrast]] || '''DSC''' || [[Gadolinium contrast]] is injected, and rapid repeated imaging (generally gradient-echo echo-planar [[T2 weighted]]) quantifies susceptibility-induced signal loss.<ref>{{cite web|url=https://radiopaedia.org/articles/dynamic-susceptibility-contrast-dsc-mr-perfusion|title=Dynamic susceptibility contrast (DSC) MR perfusion|author=Frank Gaillard et al.|website=[[Radiopaedia]]|accessdate=2017-10-14}}</ref>
| |
| − | |rowspan=3| In [[cerebral infarction]], the infarcted core and the [[penumbra (medicine)|penumbra]] have decreased perfusion (pictured).<ref name="Chen2012">{{cite journal|last1=Chen|first1=Feng|title=Magnetic resonance diffusion-perfusion mismatch in acute ischemic stroke: An update|journal=World Journal of Radiology|volume=4|issue=3|year=2012|pages=63|issn=1949-8470|doi=10.4329/wjr.v4.i3.63}}</ref>
| |
| − | |rowspan=3| [[File:Tmax by MRI perfusion in cerebral artery occlusion.jpg|100px]]
| |
| − | |-
| |
| − | | [[Dynamic contrast enhanced]] || '''DCE''' || Measuring shortening of the [[spin–lattice relaxation]] (T1) induced by a [[gadolinium contrast]] bolus.<ref>{{cite web|url=https://radiopaedia.org/articles/dynamic-contrast-enhanced-dce-mr-perfusion-1|author=Prof Frank Gaillard et al.|title=Dynamic contrast enhanced (DCE) MR perfusion|website=[[Radiopaedia]]|accessdate=2017-10-15}}</ref>
| |
| − | |-
| |
| − | | [[Arterial spin labelling]] || '''ASL''' || Magnetic labeling of arterial blood below the imaging slab, which subsequently enters the region of interest.<ref>{{cite web|url=http://fmri.research.umich.edu/research/main_topics/asl.php|title=Arterial spin labeling|website=[[University of Michigan]]|accessdate=2017-10-27}}</ref> It does not need gadolinium contrast.<ref>{{cite web|url=https://radiopaedia.org/articles/arterial-spin-labelling-asl-mr-perfusion-1|title=Arterial spin labelling (ASL) MR perfusion|author=Prof Frank Gaillard et al.|website=[[Radiopaedia]]|accessdate=2017-10-15}}</ref>
| |
| − | |-
| |
| − | | [[Functional magnetic resonance imaging|Functional MRI]] ('''fMRI''') || [[Blood-oxygen-level dependent]] imaging || '''BOLD''' || Changes in [[Oxygen saturation (medicine)|oxygen saturation]]-dependent magnetism of [[hemoglobin]] reflects tissue activity.<ref>{{cite web|last=Chou|first=I-han|title=Milestone 19: (1990) Functional MRI|url=http://www.nature.com/milestones/milespin/full/milespin19.html|publisher=''Nature''|accessdate=9 August 2013}}</ref>
| |
| − | | Localizing highly active brain areas before surgery.<ref>{{cite web|url=https://radiopaedia.org/articles/functional-mri|title=Functional MRI|author=Dr Tim Luijkx and Prof Frank Gaillard|website=[[Radiopaedia]]|accessdate=2017-10-16}}</ref>
| |
| − | | [[File:1206 FMRI.jpg|100px]]
| |
| − | |-
| |
| − | |rowspan=2| [[Magnetic resonance angiography]] ('''MRA''') and venography || Time-of-flight || '''TOF''' || Blood entering the imaged area is not yet [[Saturation (magnetic)|magnetically saturated]], giving it a much higher signal when using short echo time and flow compensation.
| |
| − | | Detection of [[aneurysm]], [[stenosis]] or [[Dissection (medical)|dissection]].<ref name=hopkins>{{cite web|url=http://www.hopkinsmedicine.org/healthlibrary/test_procedures/cardiovascular/magnetic_resonance_angiography_mra_135,14|title=Magnetic Resonance Angiography (MRA)|website=[[Johns Hopkins Hospital]]|accessdate=2017-10-15}}</ref>
| |
| − | | [[File:Mra-mip.jpg|100px]]
| |
| − | |-
| |
| − | | [[Phase contrast magnetic resonance imaging|Phase-contrast MRA]] || '''PC-MRA''' || Two gradients with equal magnitude but opposite direction are used to encode a phase shift, which is proportional to the velocity of [[Spin (physics)|spins]].<ref>{{cite web|url=https://radiopaedia.org/articles/phase-contrast-imaging|title=Phase contrast imaging|author=Dr J. Ray Ballinger et al.|website=[[Radiopaedia]]|accessdate=2017-10-15}}</ref>
| |
| − | | Detection of [[aneurysm]], [[stenosis]] or [[Dissection (medical)|dissection]] (pictured).<ref name=hopkins/>
| |
| − | | [[File:Vastly undersampled Isotropic Projection Reconstruction (VIPR) Phase Contrast (PC) sequence MRI of arterial dissections.jpg|100px]]<br>([[Vastly undersampled Isotropic Projection Reconstruction|VIPR]])
| |
| − | |-
| |
| − | |colspan=2| [[Susceptibility weighted imaging|Susceptibility weighted]] || '''SWI''' || Sensitive for blood and calcium, by a fully flow compensated, long echo, gradient recalled echo (GRE) [[pulse sequence]] to exploit [[magnetic susceptibility]] differences between tissues.
| |
| − | | Detecting small amounts of hemorrhage ([[diffuse axonal injury]] pictured) or calcium.<ref>{{cite web|url=https://radiopaedia.org/articles/susceptibility-weighted-imaging-1|title=Susceptibility weighted imaging|author=Dr Bruno Di Muzio and A.Prof Frank Gaillard|accessdate=2017-10-15}}</ref>
| |
| − | | [[File:Susceptibility weighted imaging (SWI) in diffuse axonal injury.jpg|100px]]
| |
| − | |}
| |
| − | | |
| | | | |
| | | | |
| | --[[Bruger:Jannick Brennum|Jannick Brennum]] 1. apr 2018, 11:19 (UTC) | | --[[Bruger:Jannick Brennum|Jannick Brennum]] 1. apr 2018, 11:19 (UTC) |
MR = Magnetisk Resonans
Hvordan det virker

Figur 1 T.v. uden påvirkning t.h. under det stationære B
0 magnetfelt retning

Figur 2 Et protons spind ændret væk fra B
0 af radiosignal til M
Protoner (del af atomers kerne) spinner, dvs. de roterer om egen akse. Ved magnetisk resonans skanning anvendes et kraftigt magnetfelt angivet i Tesla (T) som påvirker spindende protoner i kroppen til at spinde (mere) i magnetfeltets plan (B0) i stedet for den normale helt frie (tilfældige) orientering af protonernes spin. (Jordens magnetfelt styrke i Danmark er ca. 1/20.000 T). De kommer dog ikke til alle at spinde i magnetsfeltets plan blot mere homogent som det ses af figur 1. Med et radiofrekvens signal (radiobølge) påvirkes protonernes spind-retning (eksiteres) væk fra B0 og vinklen fra B0 vil vibrere i takt med radiosignalets frekvens og så længe protonernes spind-retning påvirkes af radiosignalet vil der generes et tilsvarende radiosignal af protonen. Der er tale om et ganske svagt radiosignal i forhold til det stationære magnetfelts styrke, men ved at gentage det samme frekvens som protoners naturlige svingningsfrekvens induceres resonans hvorved det radiosignal der udsendes forstærkes. Når radiosignalet slukkes dør det at protonen udsendte radiosignal ud over tid i takt med at protoners spind retning svinger tilbage til B0. Forestil dig et kompas hvor kompasnålen skubbes lidt at et radiosignal og vibrere i takt med radiosignalet så den ikke længere peger mod nord, og når radiosignalet slukkes og den svinger tilbage og peger mod nord dør kompasnålens radiosignal ud. Det er den uddøen af signalet relaxation & decay der måles på. I modsætning til kompasnålen opfører protonerne sig ikke som en pil, de spinder og de bliver vippet om egen spindakse og kommer til at beskrive en kegleform (Figur 2). Denne bevægelse kaldes præcession. Det er oftest protonerne i brint atomerne, som primært findes i vand molekylet der, anvendes til billeddannelse med MR-skannerer. Brintkernen, som består af en enkelt proton (og ingen neutron) er yderst velegnet til formålet, dels fordi brint findes i store mængder i humant væv (indgår som bekendt både i vand og i fedt) og dels fordi den enkelte brintkernes magnetiske moment er relativt kraftigt. I princippet kan alle atomkerner med proton-spin studeres med MR, her er nogle eksempler: ¹H, ¹³C, ²³Na og ³¹P. En og samme atomkerne vil typisk kunne antage flere forskellige spindtilstande, som hver især er karakteriseret ved et specifikt energiniveau.
Kontrasten mellem de forskellige væv og strukturer i billeder opstår ved at protonernes spind i forskelligt væv svinger tilbage med forskellig hastighed. Der anvendes forskellige standard sekvenser ved MR-skanninger, som hver har deres specialer fordele og svagheder. Disse sekvenser fremkommer ved at måle på forskellige ændringer i spin i forhold til det stationære magneltfeltsretning, samt ved at ændre på hvilken del at tilbagefaldet til protonernes spind i magnetfeltetsplan =Echo Time(TE). En anden parametre der justeres i de forskellige sekvenser er Repetition Time (TR) som er tiden mellem 2 eksitationer (radiofrekvens signaler).
Hvordan kommer vi fra spind af 1 proton til billede?
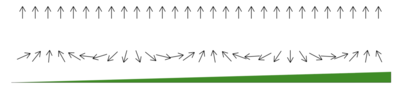
Figur 3 Foroven uden feltgradient blotB
0 forneden med feltegradient
Hvis vi ikke kan lokaliserer de enkelte protoner spind men kun et gennemsnit af det samlede hjælper det os ikke til at lave et billede af hjernen. Det næste geniale skridt var at påvirke med en magnetisk gradient (felt gradient) gennem det undersøgte væv, således at protonerne i forskellige lokalisationer har forskelligt "grundspind" som bliver deres lokalisations signatur (figur 3). Ved at skanne med forskellige feltgradienter bliver det muligt at sammenstykke et billede hvor de forskellige registrerede radiosignaler sammensættes til et detaljeret billede.
T1-vægtede billeder er baseret på ændringer i protonernes spin (rotation om egen akse)på langs af det statiske magnetfelt.
T2-vægtede billeder er baseret på ændring på tværs af det stationære magnetfelts retning. T1-vægtede billeder er særligt gode til at fremstille hjernens cortex, mens T2-vægtede billeder er særligt gode til at fremstille ødem (øget vand indhold) og inflammation.
Kontrast anvendes specielt i hjernen når man vil identificere områder hvor den normal blod-hjerne barrierer er defekt. Dette sker eksempelvis i mange tumorer, abscesser og i nogle andre infektionstilstande. Blod-hjerne barriereren skyldes at karvæggene i hjernen er særligt tætte for mange substanser som under normale omstændigheder ikke kan forlade blodbanen og komme ud i extracellulærvæsken i hjernen. Gadolinium anvendes som kontrast, dette er et paramagnetisk stof som giver tydelige signal forandringer i MR-billedet. Gadolinium ophobes i kroppen og særlig forsigtighed skal udvises hos personer med nyreskade.
De fleste MR-skannerne der rutinemæssigt anvendes i klinikken er enten 1,5 T eller 3T maskiner, men der er nu etableret en 7T maskine på Hvidovre Hospital, til forskningsbrug. Der er ingen stråling involveret i MR-skanninger. MR-skanninger blev opfundet i 1970'erne og er det mest fantastiske der er sket for neurokirurgien.
Læs meget mere her
Sekvenser
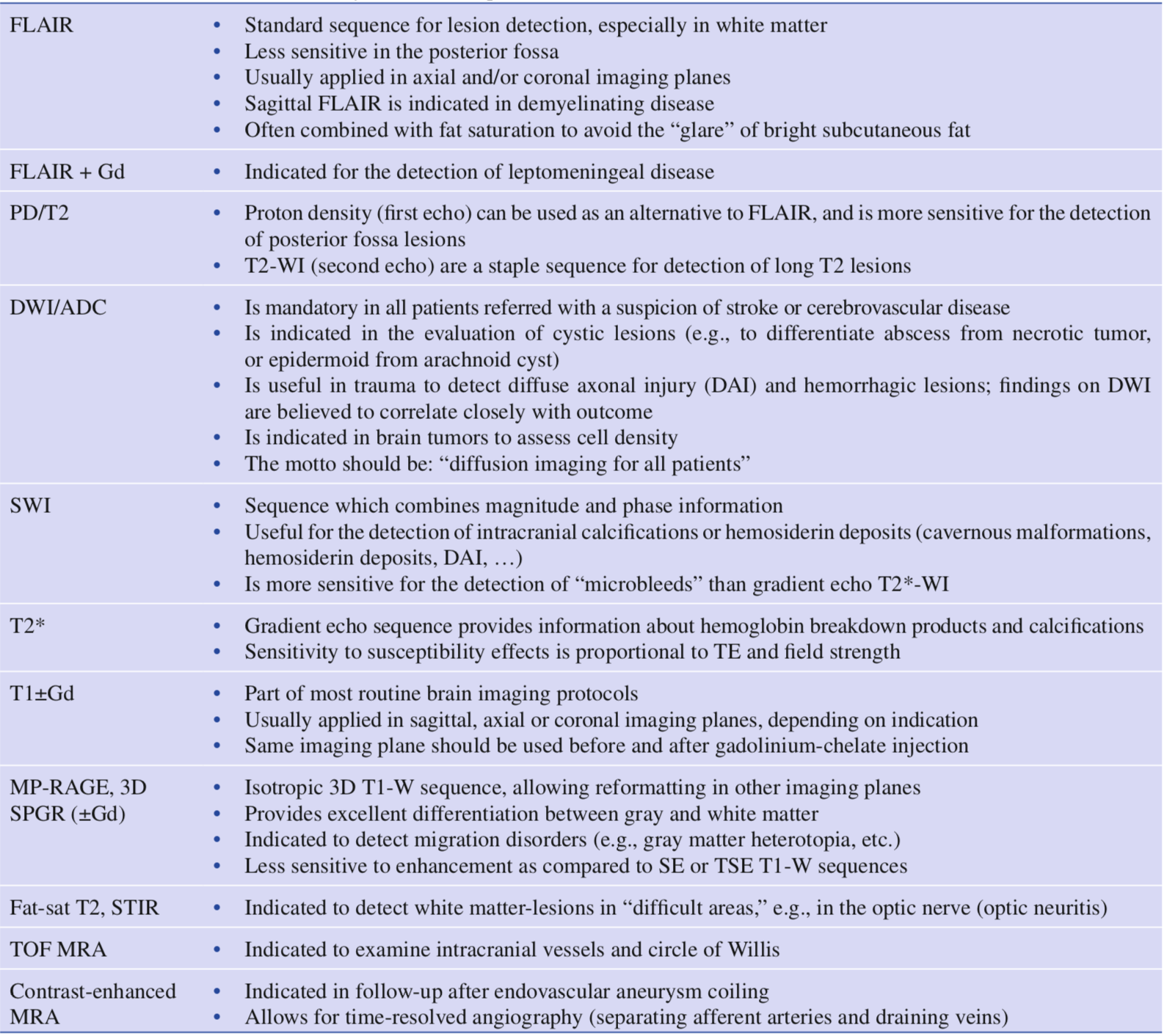
--Jannick Brennum 1. apr 2018, 11:19 (UTC)



